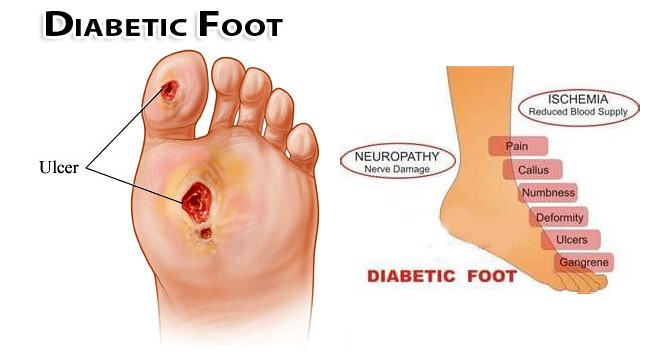
What causes a foot ulcer?
As we learned last week, a foot ulcer is a common cause of lower extremity issues for those with diabetes. They are most often found to develop in older men. The most common mechanism of injury results from repetitive and unperceived pressure on bony areas of the foot as well as pre-existing deformities.
There are many reasons a diabetic individual can develop an ulcer. However, it has been found that most diabetic foot ulcers are commonly caused by four main things.
Poor circulation
Poor blood circulation is a form of vascular disease. This means that blood doesn’t flow to your limbs efficiently (and that includes your feet, most distant from the heart). Poor circulation can also make it more difficult for diabetic ulcers to heal.
High blood sugar (hyperglycemia)
High glucose levels also slow down the healing process of an infected foot ulcer. This is one of the reasons why it’s critical to have well-managed blood sugar levels. Individuals with type 2 diabetes often have a more difficult time fighting off infections from ulcers.
Nerve damage
Nerve damage is an irreversible and long-term effect that can lead to a loss of feeling in your feet. Initially, damaged nerves can feel tingly and even painful. As nerve damage progresses it reduces your sensitivity to foot pain. This is results in painless wounds that can cause ulcers.
Irritated or wounded feet
Ulcers can sometimes be a result of improperly fitting or even inappropriate shoes. Wearing improper footwear can cause abnormal weight-bearing, areas of concentrated pressure, and abnormal shear forces on the feet. This can then increase the likelihood of experiencing foot stress.
There are three main types of ulcers.
Neuropathic Ulcers
These ulcers ccur when there is chronic repetitive trauma or friction on weight-bearing areas of the foot. These ulcers are painless and surrounded by calluses. They are located by the bony areas of the foot (specifically the toes).
Arterial Ulcers
Ulcers of this type are produced when there is a diminished flow of blood to the foot and lower leg resulting in a lack of blood supply. They are located near bony areas. Most often they occur on the tips or between toes, heels, and side or sole of the foot.
Venous Ulcers
Ulcers of this caliber develop when the deep veins of the leg fail to return blood to the heart. This causes pooling in the lower leg. Ulcers under this category typically develop on the lower leg and are most often preceded by itching and swelling.
Remember! Signs that you are experiencing foot ulcers are not always obvious. There are many times you may not show any symptoms until the ulcer has become infected. If you’re unsure, the best thing to do is talk to your doctor. This is especially important if you begin to see any skin discoloration or you begin to feel any pain around an area that appears callused or irritated.
Join us next week for a more in-depth look at how to treat a diabetic foot ulcer.
Bushby, A. (2012). Diabetes Mellitus. Clinical practice guidelines: A reference manual of best practice in pedorthic care (pp. 5-6). Winnipeg, MB: Pedorthic Association of Canada.
The Healthline Editorial Team, medically reviewed by Steve Kim, MD, (2016, February 18). Diabetic foot pain and ulcers: causes and treatment. Healthline. Retrieved from https://www.healthline.com/health/diabetic-foot-pain-and-ulcers-causes-treatments#risk-factors